Skeletal System
Intro:-
- Bone is a specialized connective tissue characterized by a min- eralized extracellular matrix. It is a highly dynamic tissue, second only to blood in its capacity for regeneration. Unlike cartilage, bone is a highly vascular. Its functions are numerous. Bones serve as scaffolds for the soft tissues of the body.
- They protect important vital organs such as the brain and heart. The bone marrow is the site for the production of cellular components of the blood. Bone tissue serves as a reservoir of calcium and phos- phorus to help maintain constant concentrations in body fluids.
- The long bones serve an important function of providing attach- ment to skeletal muscles, serving as levers for movements of the body and locomotion. This chapter will focus on the classifica- tion, general features and histology of bone tissue.
CLASSIFICATION OF BONES
Bones can be classified based on the following:
a. Position :
Bones can be part of either the axial or appendicular skeleton. The bones of the axial skeleton tendto lie along the central axis of the body and consist of the skull, vertebrae, sternum and ribs. The appendicular skele ton consists of the bones of the upper and lower limb.
b. Shape
- Depending on their shape, bones can be classified as long, short, flat, irregular or sesamoid. Long bones are seen in the upper and lower limbs. The femur and humerus are typical examples of long bones. Examples of short bones include the carpal and tarsal bones seen in the wrist and foot respectively.
- The bones forming the skull cap or calvaria like the parietal bone are examples of flat bones, along with the ribs, sternum and scapulae. Irregular bones usually have a number of projections such as the vertebrae and bones forming the skeleton of the face. Sesamoid bones form within tendons of muscles. Examples are the patella and pisiform.
c. Structure:
Lamellar bone consists of layers of bone tissue called lamellae. All bones found in adults are of this type. Lamellar bone is usually heavily mineralized and has relatively less cellular elements as compared to woven bone. Woven bone is typically seen in the developing fetus.

 Classification of bones
Classification of bonesd. Development:
Bones may either develop from membranes or cartilage. Those that develop from membranes are said to develop by intramembranous ossification. Examples include the bones forming the calvaria of the skull, such as the parietal bone. In the process of endochondral ossifica- tion, a cartilaginous model of the bone is replaced by bone tissue. This type of ossification is seen in a majority of the bones of the limbs.
TERMS USED TO DESCRIBE THE GROSS ANATOMY OF BONES
A number of terms are used to describe the gross features of bones. Some of the more commonly used terms are listed below
- Condyle-rounded articular area
- Crest-ridge
- Epicondyle-nonarticular eminence superior to a condyle
- Facet-smooth, flat area
- Foramen-hole
- Fossa – depression
- Groove-linear depression or furrow
- Line – linear elevation
- Malleolus – rounded process
- Notch-indentation
- Protuberance – projection
- Spine – thorn-like process
- Spinous process – projecting spine-like part
- Trochanter – large, blunt elevation
- Tubercle – small, raised eminence
- Tuberosity – large, rounded elevation
GENERAL FEATURES OF LONG BONES
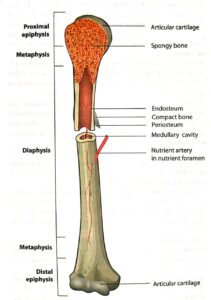
- Long bones have an upper end, a lower end and a shaft. The two ends of the bone form joints with adjacent bones. Around the ends, bones usually have muscle attachments which produce bony elevations. The shaft consists of compact bone, enclosing a marrow cavity.
- The two ends have a core of spongy bone which is covered by compact bone. The shaft or diaphysis of the bone develops from a primary centre of ossification in intrauter- ine life. The ends of long bones, called epiphyses, develop from secondary centres of ossification usually after birth.
- The growing ends of the diaphysis adjacent to the epiphysis are called metaph- yses. The metaphysis and epiphysis are separated by a cartilagi- nous epiphyseal growth plate. This growth plate is responsible for the growth in length of long bones.
- Around the time of puberty, the diaphysis fuses with the epiphyses, after which the bone cannot grow in length any further. Initially, a long bone is supplied by a nutrient artery which pierces the shaft close to the middle of the bone. Subsequently this artery is supplemented by other arteries such as metaphyseal, epiphyseal and periosteal arteries.
GENERAL MICROSCOPIC FEATURES OF BONES
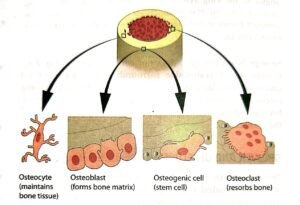
- Like other types of connective tissue, bone contains widely separated cells surrounded by large amounts of matrix. The four principal types of cells in bone tissue that have been described include osteogenic cells, osteoblasts, osteocytes and osteoclasts (Fig. 8-5).
- Osteogenic cells are resting cells that can transform into osteoblasts. They are flattened, and resemble fibroblasts and are found on the external and internal surfaces of bones (bone lining cells) as well as in growing bones. They have the capacity to divide and proliferate on stimulation. Osteoblasts are the cells that are responsible for laying down the bone matrix and are derived from osteoprogenitor cells.
- They are basophilic, roughly cuboidal cells which show all fea- tures of typical of protein secreting cells. They form a covering monolayer on the forming surfaces of growing and remodelling bone and are responsible for the synthesis of osteoid (bone matrix) and its mineralization. Once embedded in the matrix, they change to osteocytes.
- Osteocytes are long lived, amitotic cells that actively maintain the bone matrix that has already been laid down. They are smaller than osteoblasts with less cytoplasmic basophilia.
- They are mature bone cells that sit in lacunae. Stellate in shape, they possess numerous interconnected dendritic processes located within canaliculi. These serve as gap junctions between osteo- cytes, providing electrical and metabolic continuity. Osteoclasts, however, break down bone matrix by the release of enzymes that digest the bone.
- They are derived from monocytes and are mul- tinucleated, probably the result of the fusion of a number of cells. They are large, motile and polymorphic cells with a vari- able number of oval, closely packed nuclei. Located in close contact with bone, they lie in resorption bays (Howship lacunae) and have a ruffled border.
- The matrix of bone is special as it contains mineral salts that confer it with its characteristic hardness. These mineral salts are found primarily as calcium hydroxyapatite crystals. Calcium carbonate and phosphate are also seen in smaller quantities.
- These mineral deposits are seen amidst a framework of type 1 collagen fibres, which provide the bone with tensile strength. Small amounts of noncollagenous organic components like gly- coproteins and proteoglycans also contribute to the matrix.
- The periosteum is a double layered membrane covering the outer surfaces of bones. It consists of an outer fibrous layer and an inner cellular layer containing osteogenic cells. The endosteum, which lines all internal cavities of bone, is thinner and more cellular.
MICROSTRUCTURE OF LAMELLAR BONE
- Lamellar bone is the type of bone tissue found in adults. The following types of lamellar bone have been described: (1) compact bone and (2) spongy bone. Compact bone is hard and found in the shafts of long bones and outer and inner surfaces of the bones forming the skull cap or calvaria and ribs.
- It provides the structural rigidity required at these locations. Spongy bone, however, is porous and found at the ends of long bones and within bones such as the ribs. The marrow spaces in spongy bone are important sites of haematopoiesis.Skeletal System
- Compact bone is organized into osteons, also called Haversian systems (Fig. 8-6). An osteon consists of concentric lamellae arranged around centrally placed Haversian canals. Blood vessels run within the Haversian canals and serve to nourish the surrounding bone tissue. Osteocytes occupy small cavities called lacunae and are arranged along the concentric lamellae.Skeletal SystemSkeletal SystemSkeletal System
- Canaliculi connect lacunae and contain processes of osteocytes. This mechanism serves to provide intercellular communication between the osteocytes. Volkmann’s canals are situated at right angles to the long axis of the Haversian canals and serve to connect adjacent Haversian canals. Other lamellae found in compact bones include interstitial, inner and outer circumfer- ential lamellae.
- Spongy bone, however, does not contain osteons (Fig. 8-6). It consists of trabeculae surrounding red marrow-filled spaces. Trabeculae contain irregularly arranged lamellae and osteocytes connected by canaliculi. Osteoblasts line the tra- beculae, whereas osteocytes are located within the lamellae of the trabeculae.
GROWTH AND DEVELOPMENT OF BONE
- Bones ossify by two methods: intramembranous (Fig. 8-7) and endochondral (Fig. 8-8). Intramembranous ossification takes place in connective tissue membrane formed from embry- onic mesenchyme. Many skull bones, part of the mandible and the diaphysis of the clavicles are formed by this mechanism. Once ossification is complete, it is indistinguishable from endo- chondral bone.Skeletal SystemSkeletal SystemSkeletal System
- Endochondral ossification is seen in bones of the base of the skull, part of the mandible, epiphyses of the clavicles and most of the remaining bones of skeletal system. Cartilage formation begins at end of 4th week of development. Primary ossification centres start appearing at around the 2nd month of intrauterine life.
- Growth in length occurs at the epiphyseal plate which involves the formation of new cartilage by interstitial growth or appositional growth.Skeletal SystemSkeletal SystemSkeletal SystemSkeletal SystemSkeletal System
- Interstitial growth occurs from within the cartilage by proliferation of cells, whereas in apposi- tional growth, growth in diameter occurs due to addition of new bone tissue by periosteal osteoblasts. The size and shape of a bone are determined genetically but can be modified and influ- enced by nutrition and hormones. Key nutrients required for bone growth include calcium, proteins, vitamin D and vitamin C.
- Hormones such as growth hormone, sex hormones like testoster- one, calcitonin and parathormone are also critical in controlling bone growth.
APPLIED ANATOMY
- Breaks in the continuity of a bone are called fractures. When the fractured ends are exposed to the outside, it is known as a compound fracture. Otherwise it is termed a simple fracture. As the periosteum of bones receives a rich nerve supply, fractures are painful. The fractured ends can reunite if set in place, as bone has a great ability to regenerate after an injury.
- Bones are a common site of spread of malignant tumours from the prostate gland, breast and lungs. These are called bone metastasis or secondary tumours. The most common primary bone malignancy is osteogenic sarcoma.Skeletal SystemSkeletal SystemSkeletal SystemSkeletal System
- A deficiency of vitamin D causes rickets in children and osteomalacia in adults. In this condition, the mineralization of bone is affected causing bone weakness and its attendant clinical manifestations, such as bone pain, bone deformities and muscle pain.
- Abnormalities in the levels of growth hormone can affect bone growth. Excess growth hormone levels cause gigantism in children and acromegaly in adults. Decreased levels in childhood can cause dwarfism.
- Achondroplasia is a genetic disease (autosomal domi- nant) in which the growth of long bones is affected due to abnormalities in the epiphyseal growth plate of carti lage. Affected individuals have short limbs, but a normal torso.Skeletal SystemSkeletal System
- Bone marrow biopsy is done to diagnose certain types of diseases such as leukaemias and lymphomas. For this, a biopsy needle is introduced into either the hip bone or sternum, and marrow cells aspirated for further analysis.
- Bone marrow transplant involves replacing diseased bone marrow cells with healthy ones in patients with clinical conditions such as leukaemia, lymphoma and aplastic anaemia.

